What Happens if Atopic Dermatitis Is Untreated?
:max_bytes(150000):strip_icc():format(jpeg)/Health-GettyImages-2026087462-f59462f5a72546f4832837cbfbd9a930.jpg)
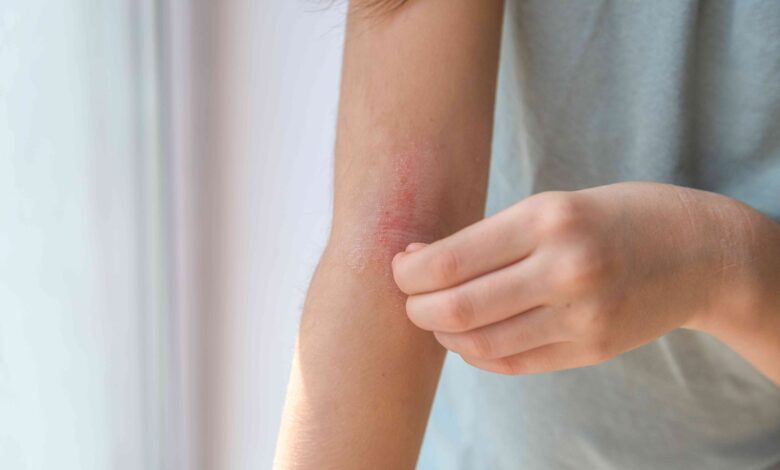
Atopic dermatitis (the most common type of eczema) causes dry, itchy skin with rough, scaly patches. It affects up to 30% of children and 10% of adults, with about 60% of cases starting before age 1.
Early treatment is important. Without it, atopic dermatitis can lead to skin infections, lasting skin changes, and mental health struggles.
Working with a healthcare provider can help you understand your triggers, manage your symptoms, and prevent complications.
When left untreated, atopic dermatitis can persist, worsen, or lead to permanent skin changes. Your skin may become thick, rough, darker, or lighter.
Untreated atopic dermatitis can also lead to the following complications:
Infections
Atopic dermatitis can cause your skin to lose moisture, acidity, and germ-fighting proteins. This can cause skin cracking, giving germs a place to enter. It also makes it easier for germs to grow, increasing the risk of infection.
The most common infection associated with atopic dermatitis is Staphylococcus aureus (staph) bacteria. More than 90% of people with eczema have this bacteria on their skin, compared to 10% of people without eczema. The infection can cause red sores that burst and form honey-colored crusts.
Staph bacteria also stick to eczema-prone skin and release toxins that break down the skin barrier further. This can lead to antibiotic-resistant infections, including methicillin-resistant Staph aureus (MRSA), which can be more aggressive in people with eczema.
Infections can sometimes spread deeper into your body and cause abscesses (painful, pus-filled lumps under the skin). More rarely, infections can spread to your blood, bone, heart, or joints.
Untreated atopic dermatitis may also make you more prone to:
- Other bacterial infections, such as Streptococcus (strep)
- Fungal infections, such as athlete’s foot or ringworm
- Kaposi varicelliform, a serious viral infection that happens when herpes infects damaged skin, causing painful blisters that spread quickly (including to skin that isn’t affected by atopic dermatitis)
- Other viral infections, such as the coxsackie virus (which causes hand, foot, and mouth disease) or molluscum contagiosum (which causes bumps on the skin)
Sleep Disturbances
The urge to scratch may be disruptive to your sleep.
Children and adults with atopic dermatitis may take longer to fall asleep, have lower sleep quality, and feel sleepier during the day. The more severe the atopic dermatitis—which is more likely if it’s left untreated—the worse the sleep troubles are likely to be.
Poor sleep may lead to other complications, as well, including:
- Decreased performance at work or school
- Worsened mood
- Worse overall health
- Personal conflicts
- Behavioral problems
- Stunted growth
Mental Health Risks
Living with atopic dermatitis can be frustrating and stressful. You might also feel self-conscious or avoid social activities, affecting your mood. About 30% of people with atopic dermatitis have been diagnosed with depression or anxiety.
If atopic dermatitis is affecting your mental health, consider talking to a counselor or support group.
Eye Complications
Severe atopic dermatitis affecting the skin near your eyes can cause eye issues such as conjunctivitis (pink eye) or keratitis (inflamed cornea). These conditions may lead to:
- Blurry vision
- Eye discomfort or irritation
- Light sensitivity
- Red, pink, itchy, or watery eyes
Besides treatment, factors that affect the severity and frequency of atopic dermatitis flare-ups (when symptoms are present) may include genetics, triggers, and age.
Genetic Factors
Atopic dermatitis, asthma, and allergies are part of the atopic triad. If one parent has any of these conditions, you have a 50% chance of developing one. If both parents have atopic conditions, your risk increases to 80%.
Up to 30% of people with atopic dermatitis also have filaggrin gene mutations. When filaggrin, a skin protein, doesn’t work correctly, your skin gets dry and irritated. It’s more likely to react to allergens, germs, or irritants, causing flare-ups and a higher risk of complications.
People with filaggrin gene mutations are seven times more likely to have four or more skin infections yearly. These mutations also increase the risk of ichthyosis vulgaris (dry, scaly skin) and keratosis pilaris (small, rough bumps).
Environmental and Lifestyle Triggers
Your symptoms may appear or worsen if you are exposed to certain triggers. Eczema triggers may include:
- Air pollutants, including cigarette smoke
- Cold or dry air
- Food sensitivities, such as to eggs, milk, peanuts, soy, or wheat
- Harsh soaps, detergents, and fragrances
- Hormone fluctuations
- Hot, humid temperatures or sun exposure
- Pollen, pet dander, and dust mites
- Rough or synthetic fibers such as wool or polyester
- Stress
Age
Atopic dermatitis may get better with age. Most people with this condition find their symptoms improve in their 20s. Until then, most people need creams or ointments to treat symptoms.
Atopic dermatitis treatment includes trigger avoidance, daily skin care, anti-inflammatory medications, and complementary treatments.
Avoiding Triggers
You and your healthcare provider can work together to identify common triggers for atopic dermatitis, such as harsh soaps, allergens, extreme temperatures, and certain foods. If food or other allergies are a concern, keeping a food diary or doing allergy testing can help pinpoint specific triggers.
Once you are more aware of what triggers your symptoms, avoiding those things may help keep symptoms under control.
Bathing and Moisturizers
Short, lukewarm baths can help with skin hydration and wash away germs and allergens to soothe itching. Use fragrance-free, gentle cleansers, and limit baths to 5–10 minutes. To reduce bacteria, add a half cup of bleach to a full tub of water 2-3 times per week. This is similar to chlorine levels in a swimming pool.
Apply a moisturizer for eczema at least twice a day. After bathing, apply your moisturizer within three minutes to lock in moisture.
Home Remedies
Home remedies can also help soothe your skin and decrease symptoms. Home remedies include:
- Apply a cool cloth to your skin for about 15 minutes
- Use aloe vera, coconut oil, or sunflower oil on your skin
- Use colloidal oatmeal in your bath or lotions
Wet Wrap Therapy
For wet wrap therapy, start by applying lotion or skin medications to your skin. Then, apply moistened gauze over the area before covering it with dry clothing. Leave it for at least two hours or overnight to help soothe skin and lock in moisture.
Experts recommend limiting this treatment to 4-7 days to protect your skin.
Diet and Supplements
Consider adding olive oil, apple cider vinegar, and manuka honey to your diet. Vitamin D supplements may also help.
Probiotics help balance good and bad bacteria. When taken during pregnancy or breastfeeding, probiotics may also reduce your infant’s risk of atopic dermatitis. Foods like yogurt, kefir, kombucha, sauerkraut, kimchi, and miso contain probiotics. You can also take supplements, but check with your provider about any supplements first.
Steroid Creams
Topical steroids applied under moisturizer are a go-to treatment. A common over-the-counter (OTC) option is Cortizone-10 (hydrocortisone). Your provider may prescribe stronger creams like Clobex (clobetasol) or Diprolene (betamethasone).
Long-term steroid use may cause side effects, so talk to your healthcare provider before using a steroid cream.
Nonsteroidal Prescription Medications
If you need steroid alternatives for your atopic dermatitis, your healthcare providers may prescribe:
- Cibinqo (abrocitinib)
- Elidel (pimecrolimus)
- Eucrisa (crisaborole)
- Protopic (tacrolimus)
- Rinvoq (upadacitinib)
Your provider may recommend oral immunosuppressants like Neoral (cyclosporine) or an injectable biologic like Dupixent (dupilumab) for severe atopic dermatitis.
Immunosuppressants calm the immune system, and biologics block specific immune responses to decrease inflammation and swelling. Dupixent also lowers the bacteria’s ability to stick to your skin, reducing your risk of infections.
Phototherapy
With phototherapy for eczema, your healthcare provider exposes your skin to controlled ultraviolet light. Providers typically reserve phototherapy for more serious cases.
See a healthcare provider if your atopic dermatitis:
- Affects your daily life
- Affects your mental health
- Causes severe itching or painful, cracked skin
- Doesn’t improve with home treatments
- Interferes with your sleep
- Keeps getting worse
It’s also important to see a healthcare provider if your skin develops signs of infection, such as increased redness, pus, swelling, and warmth. A fever may also signal infection.
Atopic dermatitis causes dry, itchy skin. If left untreated, several complications can occur.
Proper care is needed to help prevent infections, manage symptoms, and maintain your quality of life.
By recognizing triggers, following treatment plans, and working with a healthcare provider, you can manage your atopic dermatitis and reduce the risk of complications.




